Last Updated on January 30, 2024 by Hannes van der Merwe
In general, talking about the urgency for understanding the new MACRA/MIPS reporting usually results in physicians’ eyes glazing over! This topic seems to cause instant headaches! As consultants, we work hard at helping physicians to provide the best possible care. For this reason, we feel impelled to help spread the word regarding the urgency of the March deadline to submit your MIPS data to avoid reimbursement cuts in 2019.
What is MIPS? MIPS is the new Merit-based Incentive Payment System that is replacing PQRS. This new system of tracking and rewarding quality will have a direct impact on your 2019 reimbursement rates. This is a big topic to discuss! It’s important because it will affect your future reimbursement rates, but its not easy to explain due to how differently each medical practice is structured. Instead of reinventing the wheel to try and explain how to participate in MIPS and how this will affect your future reimbursement, I have found some of the best articles and resources for you and placed them all here!
- MIPS OVERVIEW (great overview of the whole program!)
- 10 things to know as you prepare for 2017 MIPS reporting
- Understanding MIPS 2018
- Quality Measures and Performance Scoring
- MACRA FAQs
THINGS TO KNOW ABOUT MACRA/MIPS
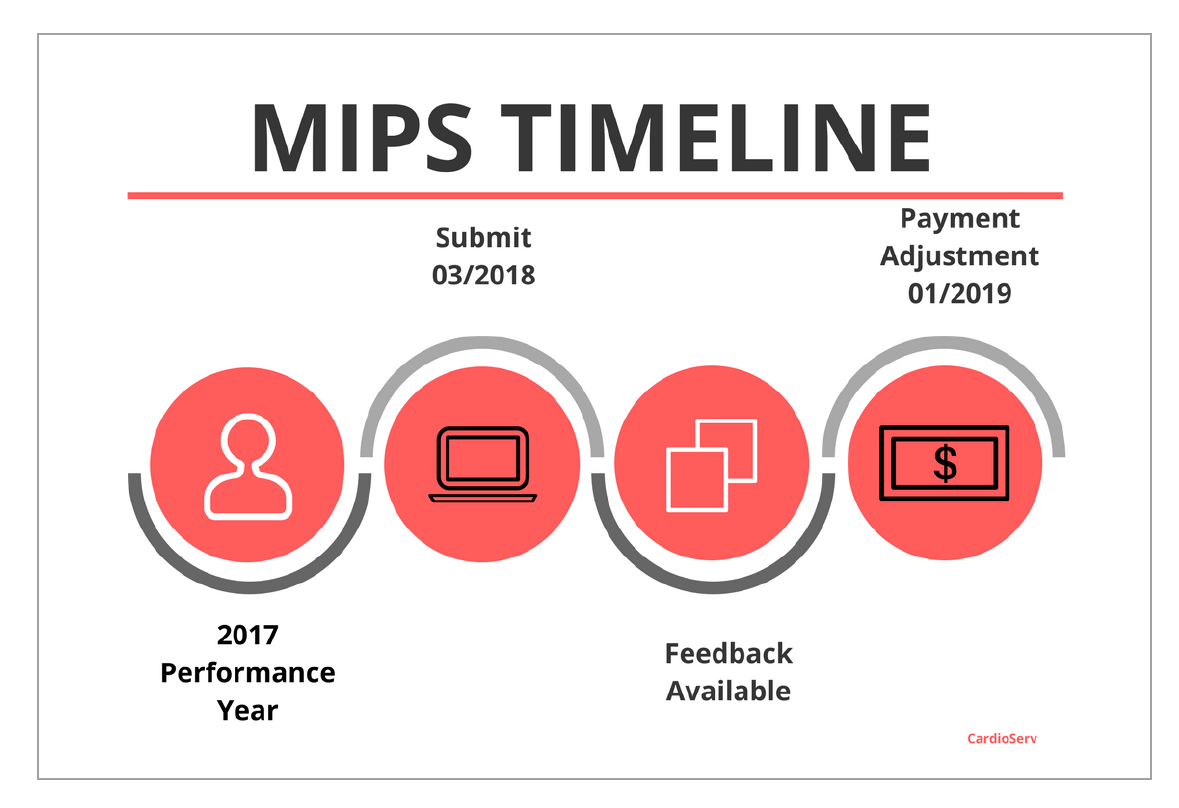
- Performance measures should have been completed in 2017
- Submission date is March 2018
- During the year you can review feedback from CMS
- 2019 payment adjustment based on your performance score
DEADLINES
- March 16, 8pm EST, is the deadline for group reporting via the CMS web interface
- March 31 is the deadline for all other MIPS reporting
3 THINGS TO DO, RIGHT NOW!
I am not kidding….
- Check the taxonomy description listed under your NPI number here
- Does your NPI number correctly identify your specialty? This can have a massive impact on future reimbursement
- Check if you need to submit data to MIPS by entering your 10-digit NPI number here
- STOP using ‘unspecified’ codes when billing!!
- Unspecified codes kill your risk score!
- List all your diagnosis codes in order of severity
- Try to list 5-6 codes per patient
ADDITIONAL RESOURCES
- The link above from the ACC, does a beautiful job of outlining quick tips for preparing for quality reporting. I suggest checking out the article which includes:
- Determine how you currently report quality to CMS
- Review your current quality performance PQRS Feedback and Quality Reports, as measured by CMS. This requires a log in that someone in your team has access to.
- Become familiar with the quality measures
- Have questions? Contact the Quality Payment Program Service Center. Email: qpp@cms.hhs.gov Phone: (866) 288-8292
- Update your physician compare data here
SUMMARY
Reimbursement is not our specialty so please seek out someone in your organization who is responsible for this important issue. Don’t ignore this…it is not going away! The good news is that although the PQRS is being phased out and replaced with MIPS, the components are similar in many ways. This means that your successful past reporting of PQRS should easily transition over to reporting under the MIPS program.

Judith Buckland, MBA, RDCS, FASE
Stay Connected: Facebook, Twitter, Instagram, LinkedIn
References:
- https://qpp.cms.gov/mips/overview
- https://www.aafp.org/journals/fpm/blogs/gettingpaid/entry/Ten_things_to_know_for_2017_MIPS_reporting.html
- https://medisolv.com/academy/part-1-understanding-mips-2018/
- https://www.acc.org/tools-and-practice-support/advocacy-at-the-acc/macra-information-hub/issue-briefs/quality
- https://www.acc.org/tools-and-practice-support/advocacy-at-the-acc/macra-information-hub/macra-frequently-asked-questions
- https://npiregistry.cms.hhs.gov/
- https://qpp.cms.gov/participation-lookup
- https://portal.cms.gov/wps/portal/unauthportal/home/
- https://qpp.cms.gov/mips/quality-measures
- https://www.cms.gov/Medicare/Quality-Initiatives-Patient-Assessment-Instruments/physician-compare-initiative/How-to-Update-your-Data-on-Physician-Compare.html