Last Updated on January 30, 2024 by Hannes van der Merwe
ARE YOU PREPARED FOR THE ICD-10
DEADLINE ON OCTOBER 1, 2015?
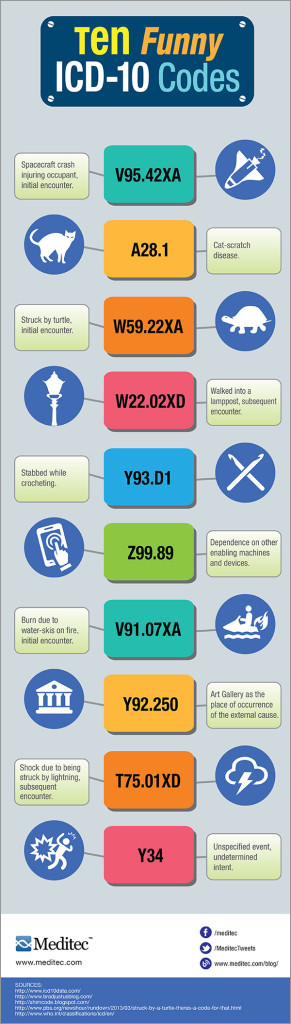
Doctors’ offices, hospitals and everyone covered under HIPPA will be making the much anticipated switch to the ICD-10 on October 1, 2015. The number of diagnostic codes will increase from 14,000 to 70,000. What does this mean for a cardiology department or office? This new coding system has the potential to better identify public health problems and manage disease and outcomes. However, under ICD-10, there will be 845 codes for angioplasty! How can cardiologists understand and be prepared for the changes? Read on for the general and cardiology specific changes occurring and how you can be ready.
 WHAT IS CHANGING?
WHAT IS CHANGING?
Here are the major ICD-10 changes:
| ICD-9-CM Diagnosis Codes | ICD-10-CM Diagnosis Codes |
| No Laterality | Laterality-Right or Left account for >40% |
| 3-5 DigitsFirst digit is alpha (E or V) or numericDigits 2-5 are numericDecimal is placed after the third character | 7 DigitsDigits 1 is alpha, Digit 2 is numericDigits 3-7 are alpha or numericDecimal is placed after the third character |
| No placeholder characters | “X” placeholders |
| 14,000 codes | 69,000 codes for more specificity |
| Limited Severity Parameters | Extensive Severity Parameters |
| Limited Combination Codes | Extensive Combination Codes for more complexity |
| 1 type of Excludes Notes | 2 Types of Excludes Notes |
(From ICD-10-CM Official Guidelines for Coding and Reporting FY 2016)
- Laterality
Some ICD-10-CM codes indicate laterality, whether the condition occurs on the left, right or is bilateral. If no bilateral code is provided and the condition is bilateral, separate codes are assigned for both the left and right side. If the side is not identified in the medical record, assign the code for the unspecified side. - Coding Digits
The ICD-10-CM has changed the coding digits. Some useful resources include: - Placeholders
The ICD-10-CM uses a placeholder character “X” for certain codes to allow for expansion. When a placeholder exists, the X must be used for the code to be considered valid. - Excludes Notes
The ICD-10-CM has two types of excludes notes. Each type of note has a different definition for use but they are all similar in that they indicate that codes excluded from each other are independent of each other.Excludes 1: A type 1 Excludes note is a pure excludes note. It means “NOT CODED HERE!” An Excludes1 note indicates that the code excluded should never be used at the same time as the code above the Excludes1 note. An Excludes1 is used when two conditions cannot occur together, such as a congenital form versus an acquired form of the same condition.Excludes 2: A type 2 Excludes note represents “Not included here”. An excludes2 note indicates that the condition excluded is not part of the condition represented by the code, but a patient may have both conditions at the same time. When an Excludes2 note appears under a code, it is acceptable to use both the code and the excluded code together, when appropriate.
HOW CAN I BE PREPARED?
Some tips for a smooth transition to ICD-10 include:
- Obtaining access to ICD-10 codes.
- Training your staff on using the new codes.
- Updating your coding processes. Examples of new key coding concepts to include on clinical documentation are:
- Laterality – left vs. right.
- Initial or subsequent encounter for injuries
- Trimester of pregnancy
- Details about diabetes and related complications
- Types of fractures
- Talk to your vendors and health plans to confirm readiness for ICD-10
- Test your systems to verify they are ICD-10 ready. You can do this by generating a claim, performing eligibility and benefits verification or coding a patient encounter.
- Medicare providers can conduct acknowledgement testing with Medicare Administrative Contractors (MACs) until October 1, 2015 to confirm that Medicare can accept the ICD-10 claims.
- If your systems are not ready, there is free billing software offered by every MAC website and paper claim providers for those meeting the Administrative Simplification Compliance Act Waiver.
FOR CARDIOLOGY, THERE HAVE BEEN THREE CATEGORIES OF CHANGES:
Source: CMS Primer to Cardiology
- Definition changes:
- Acute Myocardial Infarction (AMI) is now considered “acute” for 4 weeks from time of incident. (ICD-9 period was 8 weeks). ICD-10 does not use episode of care and allows coding of new MI occurring during the 4 week “acute period.”
- Hypertension is defined as essential (primary). There is no longer the concept of benign or malignant. When documenting hypertension, be sure to include: type and casual relationship.
- Terminology differences:
- Congestive heart failure documentation matches types of CHF. Be sure to include acuity and type.
- Underdosing is a new concept and term in ICD-10. It identifies if the patient is taking less of a medication than is prescribed. Be sure to include:
- Intentional, Unintentional, Non-compliance: Is the underdosing deliberate?
- Reason: Why is the patient not taking the medication?
- Atherosclerotic Heart Disease with Angina Pectoris documentation must include the following:
- Cause
- Stability
- Vessel
- Graft involvement
- Increased specificity:
- Cardiomyopathy documentation must include where appropriate:
- Type
- Location
- Cause
- Cardiomyopathy seen in other diseases should be listed
- Heart Valve Disease is assumed to be rheumatic; if not notate otherwise. Documentation should include the following:
- Cause
- Type
- Location
- Arrhythmias/Dysrhythmias documentation should include:
- Location
- Rhythm Name
- Acuity
- Cause
- Cardiomyopathy documentation must include where appropriate:
HOW TO ACCESS LOCAL COVERAGE DETERMINATION (LCD) FOR TEE AND TTE WITH ICD-10 CODES
- Click here to start your search.
- Select “Local Coverage”
- Select one of three display options for LCDs: LCDs by Contractor, LCDs by State or LCDs listed Alphabetically
- If you select LCDs by Contactor, then select your MAC.
- In document types, check Active LCDs.
- Click submit button and select next/previous to search pages for Transthoracic Echocardiography (TTE) and Transesophageal Echocardiography (TEE).
OTHER USEFUL CARDIOLOGY RESOURCES
- CMS’s Road to 10 Cardiology Clinical Scenarios
- Specialty Specific Training Webinars
- Clinical Concepts of Cardiology
- Build your Action Plan
ECHO SPECIFIC RESOURCES
- ASE Conversion of Select ICD-9 Codes to ICD-10
- ASE Common ICD-10 Diagnosis Codes for TEE
- ASE Common ICD-10 Diagnosis Codes for TTE and Stress Echo
- The ASE is also providing its members with complimentary access to a coding reimbursement expert and will have a webinar on ICD-10 Implementation this November.
Important note: Medicare officials say they will not deny claims for lack of specificity for 12 months, as a grace period to adapt to the new coding. However, this doesn’t apply to hospital procedure codes and you should check with commercial insurers, as they may not be offering this grace period.