Last Updated on January 30, 2024 by Hannes van der Merwe
PATIENT CENTERED IMAGING
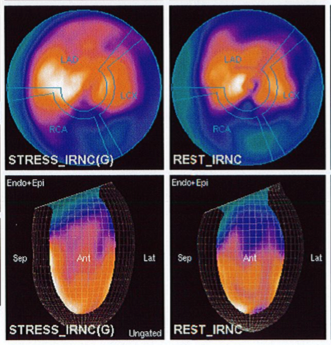
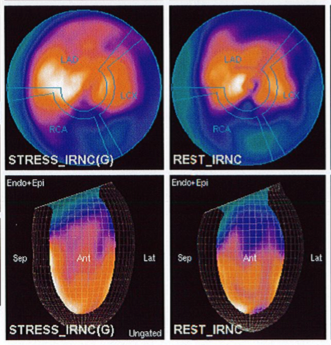
In recent years, there has been a large increase in the role of diagnostic imaging in the medical industry and with that has come increased radiation exposure. Many professional organizations have come together, including ASNC, AHA and IAC to address the issue of radiation exposure and how we can maximize the quality of diagnostic studies and patient safety while reducing radiation risk. March is Radiation Safety Month for CardioServ and we want to bring awareness of patient centered imaging. Success of nuclear cardiology is based on (1) education of clinicians and patients and (2) optimization of patient care through appropriate use criteria and proper imaging procedure for the individual patient.
EDUCATION
The foundation of improving radiation safety and moving toward patient centered imaging is education. All healthcare providers must understand which cardiac imaging tests use radiation and the associated risks. Healthcare providers performing the cardiac imaging should be up to date on the most recent advancements in radiation safety and dose optimization techniques. It is important for them to be aware of the most recent standards and guidelines provides by ASNC, ACC and AHA
There is also a need for the patient and public to understand what is involved in the cardiac imaging procedure as well as any benefits, risks and alternatives. There is public anxiety in regards to radiation and the risk of cancer. Because of this, it is important to create a dialogue with your patient and family members. Make them understand that the benefits of having the cardiac imaging performed outweighs the risk. Compare the risk estimates using comparisons they will understand.
APPROPRIATE USE AND INDIVIDUAL PATIENT OPTIMIZATION
Always apply appropriate use criteria. When clinically appropriate, the benefits of an accurate diagnosis outweigh the potential risk of radiation exposure. Myocardial Perfusion Imaging (MPI) has the most clinical utility in patients with intermediate CAD risk, those requiring prognostic or management information and those with persistent and unexplained symptoms. For younger patients, consider other modalities with comparable diagnostic accuracy but less or no radiation. Avoid repetitive testing.
Patient safety is the upmost concern when contemplating diagnostic imaging. The clinician should weigh the risk of radiation exposure individually for every patient and apply proper imaging protocols. For SPECT imaging, there are a variety of protocols to tailor to an individual person. ASNC’s Patient Centered Imaging paper offers a variety of 1 day, 2 day, stress/rest and rest/stress protocols as well as patient-specific examples on how to approach a patient from an imaging perspective to obtain a meaningful test while maximizing safety and minimizing cost.
Exercise testing is preferred over pharmacologic stress testing in patients who are able to exercise.
5 WAYS TO REDUCE RADIATION EXPOSURE:
- Perform the stress portion of the test first, review the images and determine whether the rest portion is necessary.
- Use radionuclides with shorter half-life such as Tc-99m.
- Use weight based dosing
- Use the newest software that can optimize images while lowering radiation dose.
- Use newer hardware methods that provide better quality images with reduced time and radiation dose.
In next week’s blog, CardioServ will talk about patient centered imaging and nuclear accreditation. In addition, we will elaborate more on new software and hardware methods for optimizing patient centered imaging.
RESOURCES
- ASNC Imaging Guidelines for SPECT nuclear cardiology procedures: Stress, protocols, and tracers
- ASNC Preferred Practice Statement: Patient-centered Imaging
- ASNC Information Statement: Recommendations for reducing radiation exposure in myocardial perfusion imaging
- AHA Scientific Statement: Approaches to Enhancing Radiation Safety in Cardiovascular Imaging