Last Updated on January 31, 2026 by Judith Buckland, MBA, RDCS, FASE
With the release of updated ASE diastolic function recommendations in 2025, the emphasis has shifted from interpreting individual parameters in isolation to applying structured algorithms that integrate multiple measurements. The parameters discussed below remain physiologically relevant, but their diagnostic weight depends on the clinical context and how they are used within the ASE-recommended framework.
DETERMINING LV FILLING PRESSURES
We are able to determine if the LV filling pressures are elevated or not by determining the left atrial pressure (LAP). There are various terms that describe elevated LV filling pressures: elevated LAP or elevated LVEDP. It is common for these terms to be used in conjunction with each other but all referring to the same concept: ventricle being unable to fill properly at a low pressure state, causing an increase in end-diastolic pressures in response to a stiff, non-compliant ventricle.
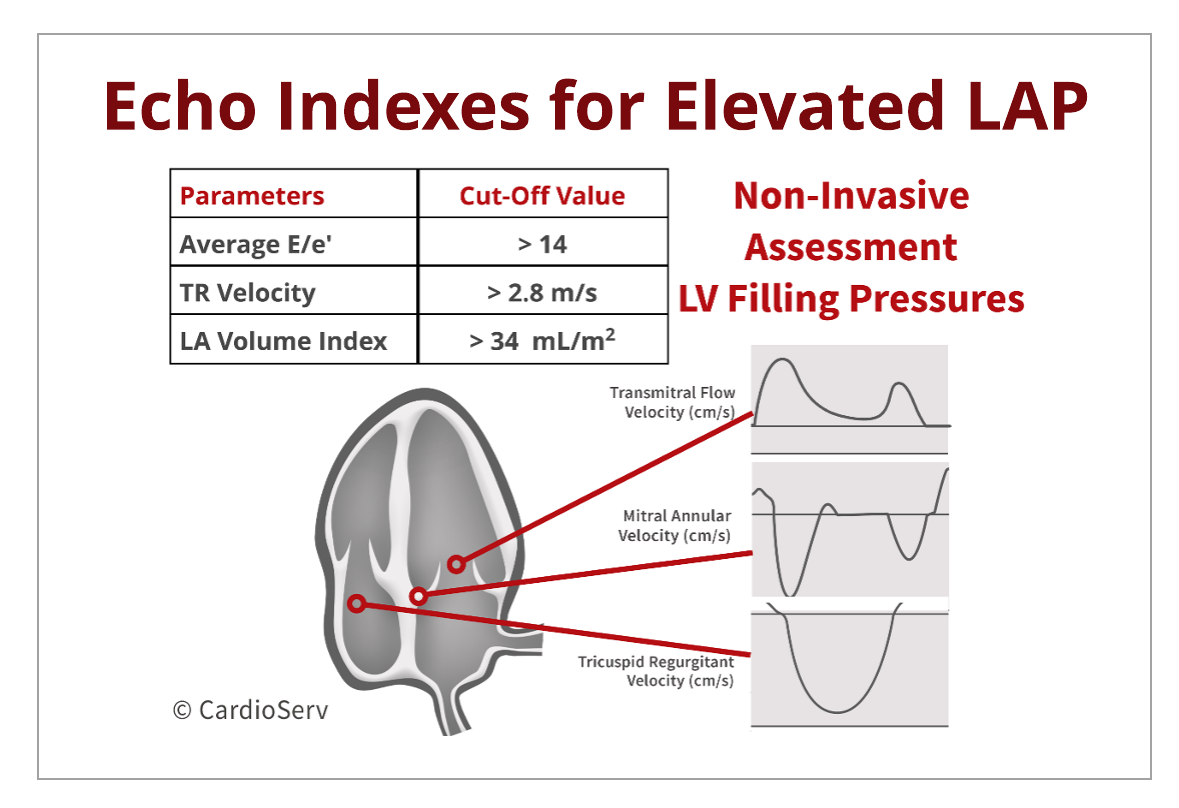
Echocardiography is unable to directly measure LV filling pressures. Instead, we use a combination of indexes. Since LAP correlates to the invasively-obtained LVEDP, we can evaluate a series of measurements to help us determine if the LAP is elevated or not.
- Tricuspid Regurgitation Velocity
- Transmitral E-Wave Peak Velocity
- E/e’ Ratio
- Left Atrial Volume Index (LAVI)
- Ar/A Duration
- E-Wave Deceleration Time (DT)
NOTE: The goal of this blog is to have a basic understanding of how these individual indexes play physiological role in elevated LAP. The ASE provides two algorithms to use in conjunction with other indexes to determine both grade of diastolic dysfunction and presence of elevated LAP. Please refer back to our guest speaker blogs to view this information.
TRICUSPID REGURGITATION VELOCITY
TR velocity provides an important indirect estimate of elevated left-sided filling pressures, particularly when pulmonary vascular disease is excluded. An elevated PAP is strongly suggestive of an elevated LAP. The presence of mitral regurgitation, which can elevate the PAP, must be taken into consideration when using this method as an indicator of LAP.
Echo can calculate this pressure by adding the peak systolic tricuspid regurgitation velocity and right atrial pressure (RAP). Refer back to our prior blog that explains how to obtain these values. A peak TR velocity > 2.8 m/s is suggestive of elevated LAP.
TRANSMITRAL PEAK E-WAVE VELOCITY
In current ASE algorithms, peak E-wave velocity is not used in isolation to determine LAP, but rather interpreted in conjunction with other diastolic parameters.
The transmitral pressure gradients (PG) determine the peak E-wave velocity, and can be used as an index for estimating LAP.
We are unable to take the peak E-wave velocity and transform it into a transmitral PG due to the true PG exceeding the predicted gradient with the Bernoulli’s equation. Therefore by measuring the peak E-wave velocity, which is the peak filling rate, we can correlate that value with the overall transmitral PG.
The LAP is the sum of the LV diastolic pressure and transmitral pressure difference. Therefore a limitation to using E-wave velocity as an index for LAP is the velocity reflects only the AV pressure difference. This is why we cannot use the peak E-wave velocity as the only parameter for determining the LAP.
E/E’ RATIO
Recent ASE guidance emphasizes that E/e′ should be interpreted cautiously, particularly in patients with regional wall motion abnormalities, mitral valve disease, or preserved EF, and should not override discordant findings.
The E/e’ ratio can be a useful parameter when used in combination of other measurements. A high E/e’ ratio is suggestive of elevated LVEDP. This method is useful because it is not effected by age and is a strong supporter of the presence of diastolic dysfunction. E/e’ ratio > 14 is considered abnormal.
The reason the E/e’ ratio is only useful in combination of other methods is due the wide normal range of the e’ value and specific limitations to e’.
LEFT ATRIAL VOLUME INDEX (LAVI)
LAVI a marker of chronic elevation in filling pressures rather than an acute indicator.
By measuring the left atrium volume and indexing it to the patients BSA, it can provide valuable information about the LAP. As LV filling pressure progressively elevate, the LAVI size will enlarge. Therefore, an enlarged LAVI is a marker of elevated LAP. In contrast, a small or normal LAVI is suggestive of normal LAP. The abnormal cut-off value for LAVI is > 34mL/m².
This measurement is not an index of determining the LVEDP because the atrium will not enlarge immediately once pressures elevate. It’s also good to note, even when LVEDP become normalized, the size of the left atrium may continue to be enlarged. That is why we cannot use the LAVI size as a direct index of determining the LAP.
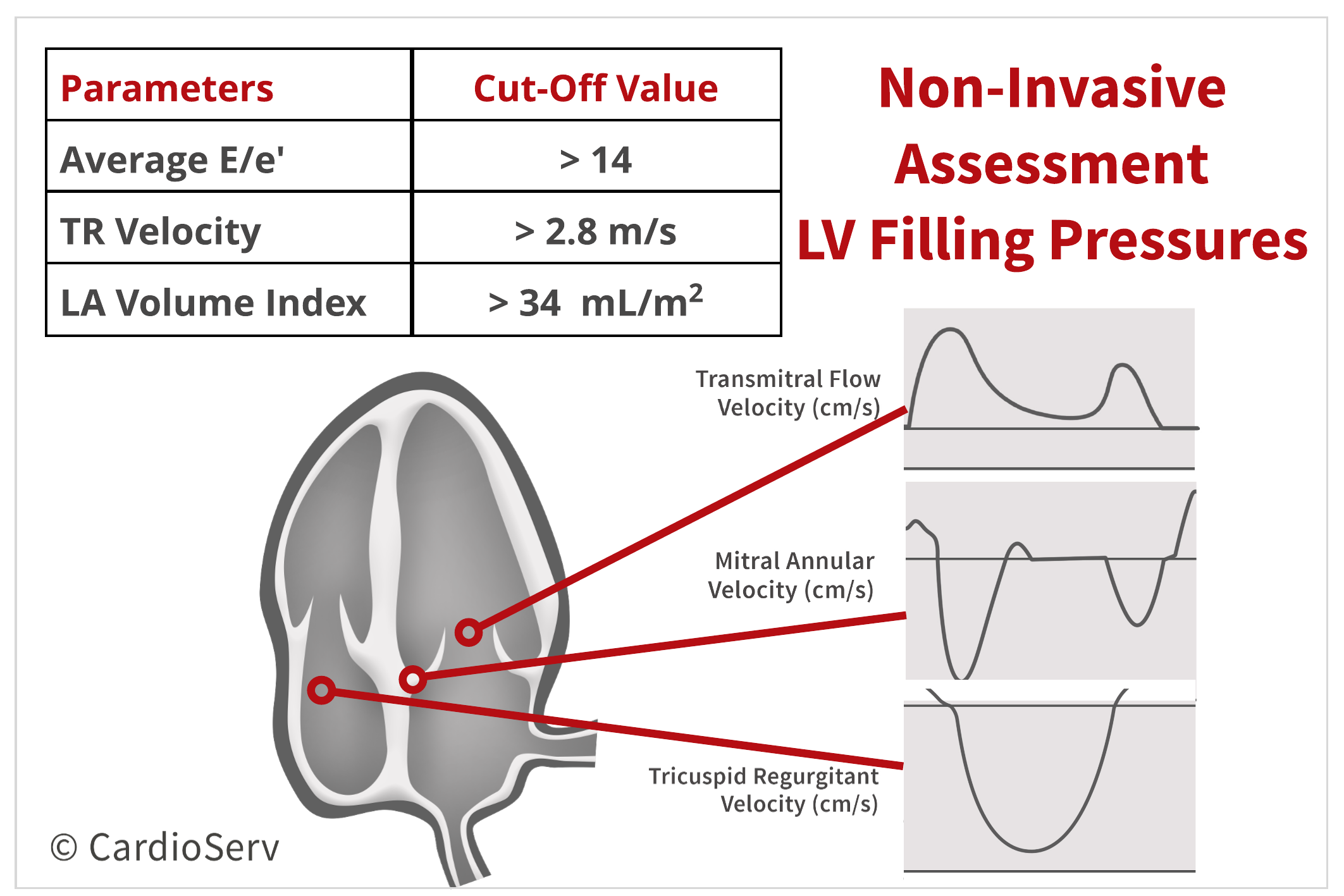
AR/A DURATION
Pulmonary venous Doppler parameters can provide supportive insight into left ventricular filling pressures when technically feasible, but they are no longer considered primary determinants in current ASE diastolic function algorithms.
Atrial Reversal (AR) Duration
The comparison of the pulmonary venous atrial reversal (AR) duration to the transmitral A-wave duration reflects left atrial contraction against a non-compliant left ventricle. An AR duration exceeding the transmitral A-wave duration by more than 30 ms has historically been associated with elevated LV end-diastolic pressure.
While this relationship remains physiologically valid, current ASE guidance emphasizes that AR duration should be interpreted as a supportive parameter rather than a standalone indicator of elevated filling pressures. Limitations include technical feasibility, signal quality, heart rhythm, and variability in acquisition, which may reduce reproducibility in routine practice.
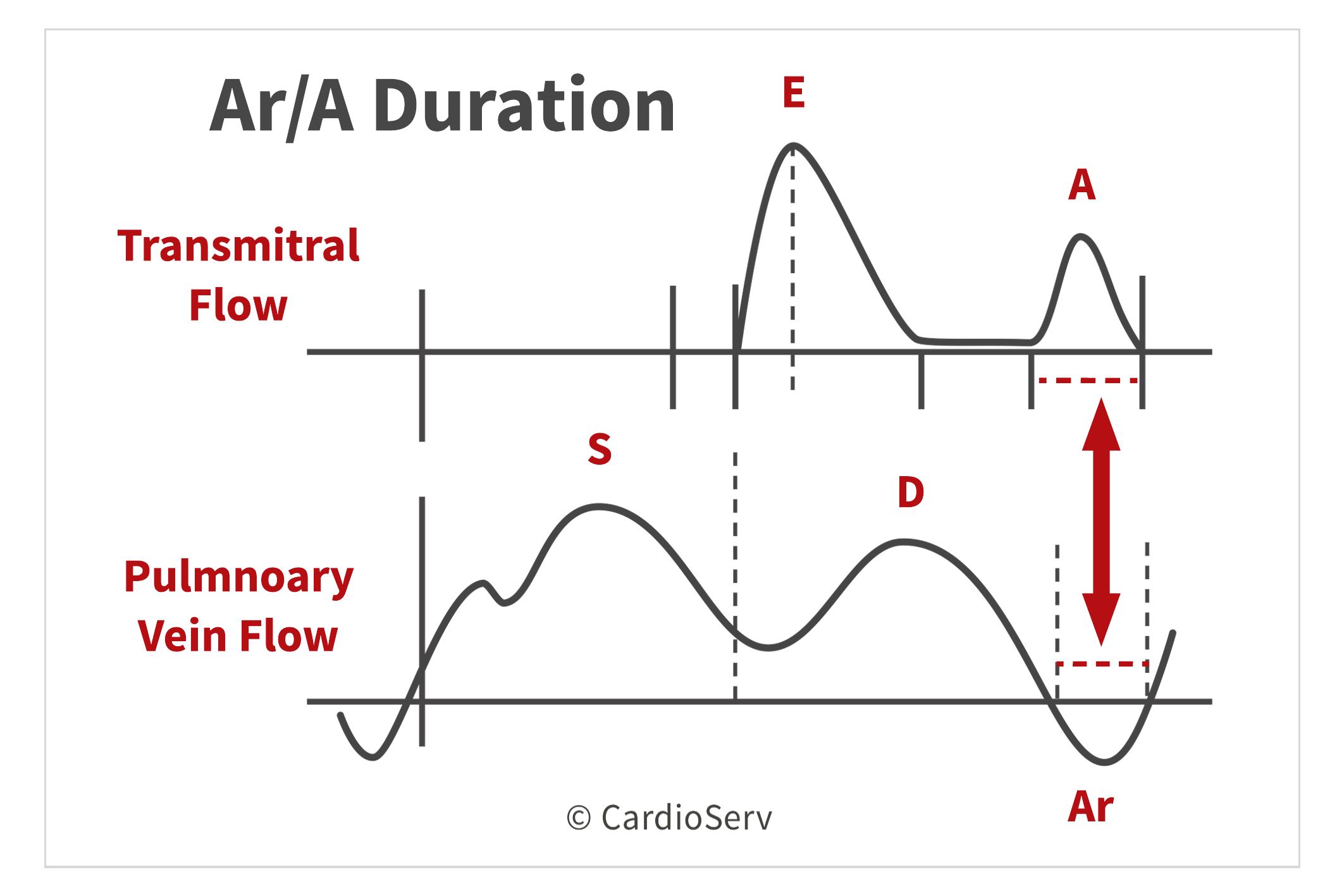
Pulmonary Venous S/D RATIO
The systolic-to-diastolic (S/D) ratio of pulmonary venous flow may provide additional context regarding left atrial pressure, particularly in patients with reduced left ventricular ejection fraction. An S/D ratio < 1 has been associated with elevated filling pressures in select populations.
However, similar to AR duration, the S/D ratio is now considered an adjunctive finding rather than a primary criterion in ASE diastolic assessment algorithms. Its interpretation should be integrated with other echocardiographic parameters and the overall clinical context.
Clinical Perspective
Pulmonary venous Doppler remains a valuable tool in experienced hands and can enhance confidence when findings are concordant with other indices. However, current ASE recommendations prioritize algorithm-based assessment using parameters with greater feasibility and reproducibility, reserving pulmonary venous measurements as complementary data points rather than required components.
DECELERATION TIME (DT)
The deceleration time of the transmitral E-wave can be an additional tool because it reflects the ventricles relaxation and filling pressures. A short DT will be due to an increased E-wave velocity, which is caused by an elevated LAP but should be interpreted in the context of other diastolic parameters and clinical findings, as it is sensitive to loading conditions and heart rate.
OTHER PARAMETERS
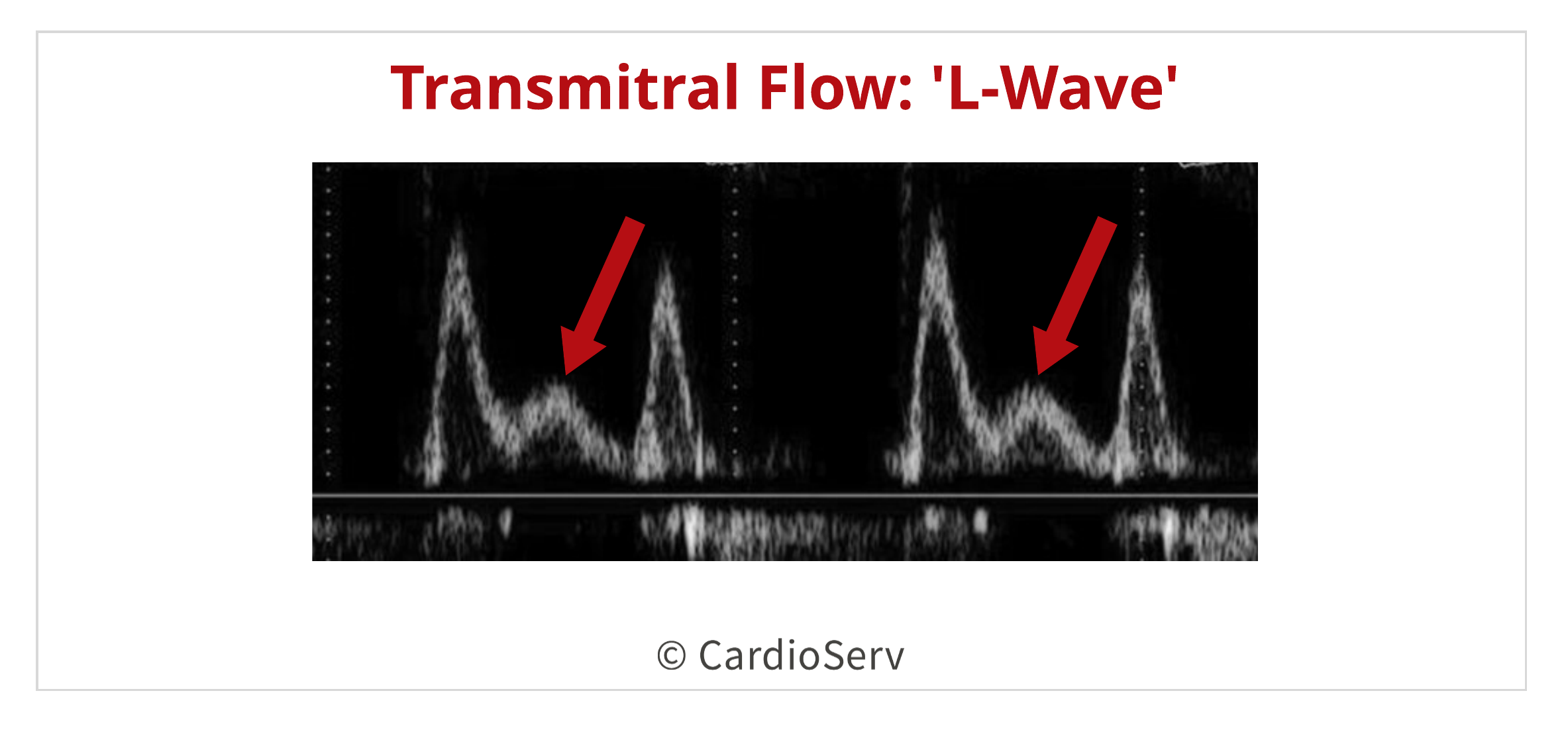
The presence of a transmitral L-wave can be an additional sign of elevated LAP. The presences of this additional wave is caused by the pulmonary vein’s A-wave flow duration occurring longer into late diastole when there is impaired or prolonged LV relaxation present. This changes the normal biphasic transmitral flow into a triphasic display.
These findings are supportive and may be helpful in experienced hands but are not required for routine diastolic classification.
Another sign of an elevated LAP, is the delayed occurrence of the e’ velocity in comparison to the E-wave velocity. This delay in occurrence is telling us that the volume of blood is being pushed into the ventricle, instead of normally being pulled via a suction due to pressure gradient changes between chambers. This comparison is done when obtaining the E-wave and e’ velocity at the same time. Certain machines offer this feature of obtaining dual Doppler recordings simultaneously.
SUMMARY
Current ASE diastolic function guidelines emphasize the use of structured algorithms that integrate multiple echocardiographic parameters rather than reliance on individual measurements. While the parameters discussed above remain physiologically relevant, their diagnostic weight depends on how they are applied within the recommended framework and clinical context.

Andrea Fields MHA, RDCS
Stay Connected: LinkedIn, Facebook, Twitter, Instagram
References:
Gillebert, T. C., Pauw, M. D., & Timmermans, F. (2013). Echo-Doppler Assessment of Diastole: Flow, Function and Hemodynamics. Education in Heart, 99, 55-64. Retrieved November 20, 2017, from https://pdfs.semanticscholar.org/deda/8ed40076f7bbb1da2668d190d15af9947c2d.pdf.
Nagueh, S. F., MD, Smiseth, O. A., MD, & Appleton, C. P., MD. (2016). Recommendations for the Evaluation of Left Ventricular Diastolic Function by Echocardiography: An Update from the American Society of Echocardiography and European Association of Cardiovascular Imaging. American Society of Echocardiography, 29(4), 277-314. Retrieved October 31, 2017, from http://asecho.org/wordpress/wp-content/uploads/2016/03/2016_LVDiastolicFunction.pdf
Andersen, O. S., MD, Smiseth, O. A., MD, & Dokanish, H., MD. (2017). Estimating Left Ventricular Filling Pressures by Echocardiography. Journal of the American College of Cardiology,69(15), 1937-1948. Retrieved November 29, 2017.
Mitter, S. S., MD, Shah, S. J., MD, & Thomas, J. D., MD. (2017). A Test in Content: E/A and E/e’ to Assess Diastolic Dysfunction and LV Filling Pressures. Journal of the American College of Cardiology,69(11), 1451-1464. Retrieved November 29, 2017.
Mottram, P. M., & Marwick, T. H. (2005). Assessment of Diastolic Function: What the General Cardiologist Needs to Know. Heart British Cardiovascular Journal,91, 681-695. doi:10.1136