Last Updated on January 30, 2024 by Hannes van der Merwe
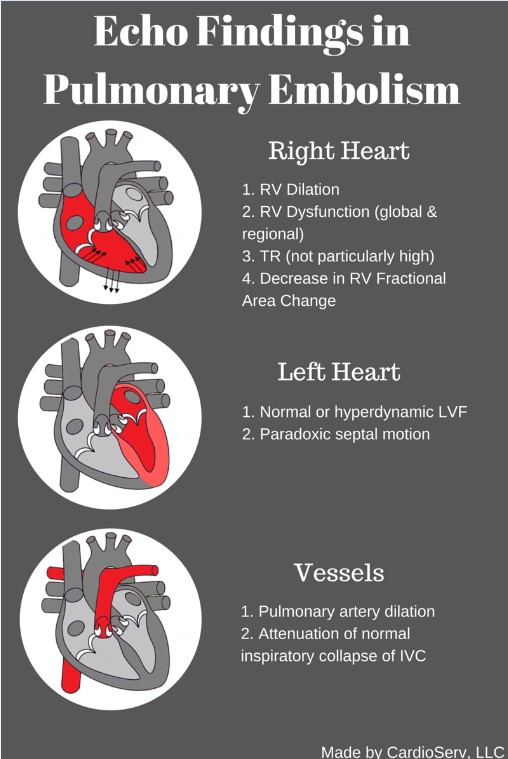
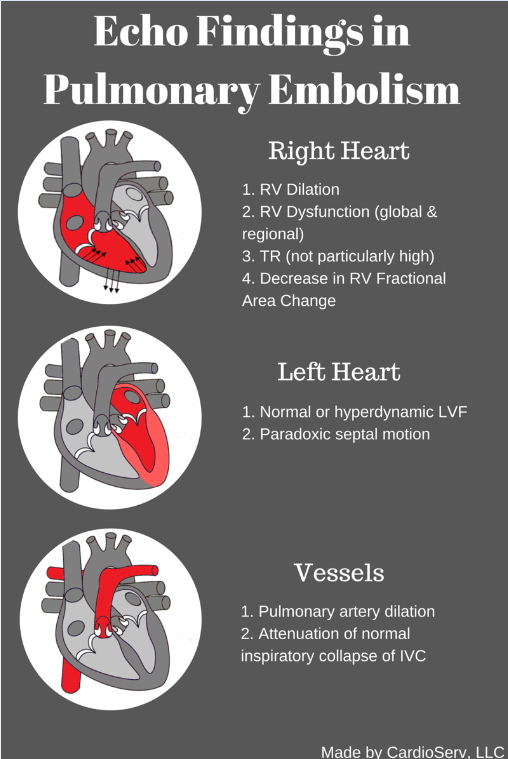
ECHOCARDIOGRAPHY IN THE DIAGNOSIS OF PULMONARY EMBOLISM
Pulmonary embolism continues to cause at least 60,000 deaths per year in the United States according to CDC statistics. Ten percent of symptomatic pulmonary emboli are fatal within one hour of symptoms onset. However, diagnosis can often be difficult because the presenting signs and symptoms are nonspecific and often mimic other cardiac and pulmonary diseases. Interventional strategies to remove or dissolve thrombi continue to improve. With these improvements, our ability to understand and diagnose also needs to improve. Echocardiography can aid in the diagnosis of pulmonary embolism and provides important functional information about the right and left ventricle that cannot be ascertained from other tests.
VISUALIZATION OF THROMBUS
The thrombus can form anywhere in the venous system and be visualized anywhere en route to the lungs (IVC, SVC, RA, RV, PA). Remember thrombi visualized proximal to PA are not diagnostic of PE but points to the process. There are also differential diagnosis of thrombi to keep in mind such as tumors or myxomas.
ASSESSMENT OF RV SIZE AND FUNCTION
Healthy Right Ventricle
A normal right ventricle (RV) is accustomed to very low pulmonary resistance. RV pressures are low and compliance is high. Unlike the left ventricle (LV), the right ventricle is not use to a lot of pressure or resistance and does a poor job at acutely responding to sudden increase in afterload. RV is an important barometer to what is happening in the pulmonary arteries and on the left side of the heart.
Right Ventricle in Pulmonary Embolus
In a pulmonary embolus, there is an acute rise in pulmonary resistance. The pulmonary pressures DO NOT go up acutely. It is a common misconception that they do.
The increase in pulmonary vascular resistance results in increased RV afterload and increased RV wall tension. The RV dilates acutely and can become dysfunctional. Reduced cardiac output leads to reduction in LV output and ultimately hypotension. Depending on the size of PE, this can result in right ventricular failure.
Pulmonary embolism → Increasd pulmonary resistance → Increased RV afterload → RV Dilatation/Dysfunction → Decreased RV cardiac output → Decreased LV preload → Decreased LV output → Hypotension
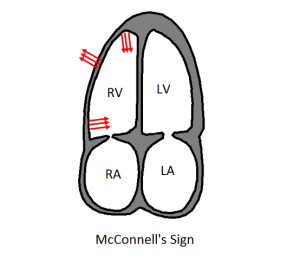
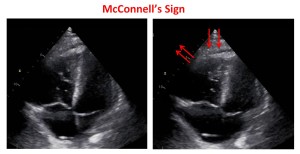
MCCONNELL’S SIGN OR ACUTE REGIONAL RV DYSFUNCTION
McConnell’s sign is one of the most distinct echocardiographic findings in patients with acute pulmonary embolism. The sudden pressure overload on the RV also causes increased wall stress. As a result, it is left mechanically stunned. The right ventricle has a complex shape: distribution of this stress is not uniform, there is mid right ventricle free wall bulging and localized ischemia of free wall due to increased stress. The apical section of the RV is not exposed to this stress due to its location next to the LV. RV apex is anatomically tethered with LV apex. The LV is usually hyperkinetic due to tachycardia and this pulls the RV apex along with it for a proxy contraction.
 |  |
TRICUSPID REGURGITATION
Remember that pulmonary resistance, not pressure, elevates during a pulmonary embolism. Therefore, TR velocities are not particularly high in an acute PE. Velocity between 2.5-3.0 m/s is normal for an acute PE assuming the right heart is not accustomed to high pressures previously.
ECHO TO ASSESS THERAPY
Echo is an effective way to monitor thrombolytic therapy. Within several hours after thrombolytic therapy or suction embolectomy, echo demonstrates:
- Reversal of RV size back to normal
- Reversal of RV dysfunction back to normal
- Can be quite dramatic
Sign up for our weekly newsletter to receive our blog and case studies directly into your inbox!
Next week we will discuss pulmonary hypertension and the differences between PH and PE in echocardiography.
Special thanks to Dr. Scott Solomon, Professor of Medicine at Harvard Medical School for your awesome Illustrative Case Presentation at the 2012 ASE Scientific Sessions – your presentation really helped explain and demonstrate pulmonary embolism in echocardiography.
Like this article? Tell us on Facebook!